Billing for Mental Health Therapists in the USA: Complete Guide to Accurate Claims, Coding, and Revenue Growth
Mental health practices across the United States are growing rapidly as awareness around behavioral health continues to expand. However, while therapists focus on patient care, managing insurance claims, coding requirements, and reimbursement policies can become complex. This is where billing for mental health therapists becomes an essential operational component for sustaining a successful practice.
Mental health billing differs significantly from traditional medical billing because it involves specialized codes, therapy session documentation, and payer-specific rules. Therapists, psychologists, psychiatrists, and counseling centers must ensure accurate claim submissions, compliance with regulations, and proper reimbursement from insurance providers.
Understanding how billing for mental health services works can help therapists avoid revenue loss, reduce claim denials, and maintain steady cash flow.
Why Mental Health Billing Is More Complex Than Standard Medical Billing
Several factors make billing for mental health providers more complicated than other medical specialties. Therapists must deal with session-based billing structures, insurance authorization requirements, and evolving coding standards.
Some of the common challenges include:
• Complex CPT and diagnosis codes used in coding and billing for mental health services
• Strict documentation requirements for therapy sessions
• Frequent claim denials due to authorization issues
• Changing payer rules for billing Medicare for mental health services
• Credentialing delays for new therapists
Because of these challenges, many practices rely on behavioral & mental health billing services that specialize in psychiatric and therapy billing processes.
Key Components of Billing for Mental Health Therapists
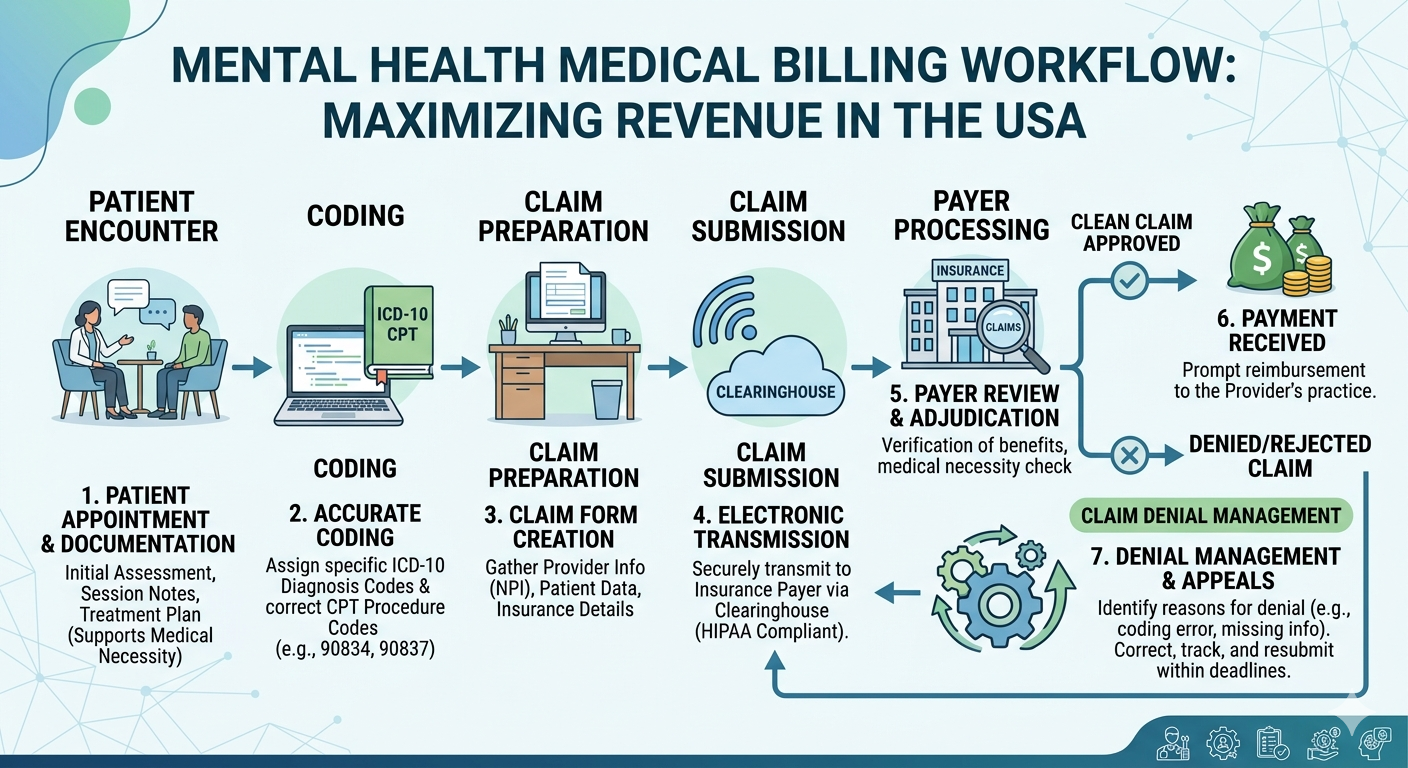
A successful billing process requires a structured workflow that begins before the patient visit and continues until reimbursement is received.
Patient Eligibility Verification
Before a therapy session begins, insurance eligibility must be verified. This step ensures the patient’s mental health benefits are active and helps determine coverage limits.
Accurate Coding and Documentation
Medical billing for mental health relies heavily on CPT codes for psychotherapy, psychiatric evaluations, and medication management. Proper documentation is essential to justify each billed service.
Claims Submission
After coding is completed, claims are submitted to insurance payers. A mental health billing company typically uses clearinghouses to transmit claims quickly and accurately.
Payment Posting
Once the insurance company processes the claim, payments are recorded and patient balances are updated.
Denial Management
Denied claims must be reviewed and corrected immediately. Mental health billing solutions often include dedicated teams that manage appeals and resubmissions.
Common CPT Codes Used in Mental Health Billing
Understanding CPT codes is essential for billing mental health services correctly. Some frequently used codes include:
90791 – Psychiatric diagnostic evaluation
90832 – Psychotherapy, 30 minutes
90834 – Psychotherapy, 45 minutes
90837 – Psychotherapy, 60 minutes
90846 – Family therapy without patient present
90847 – Family therapy with patient present
Correct coding ensures proper reimbursement and reduces claim rejection risks.
Medicare Billing Rules for Mental Health Services
Therapists working with Medicare patients must follow specific billing regulations. Billing Medicare for mental health services requires strict adherence to documentation and treatment guidelines.
Key considerations include:
• Approved provider types such as psychiatrists, clinical psychologists, and licensed clinical social workers
• Use of correct psychotherapy codes for session length
• Documentation of medical necessity
• Compliance with Medicare reimbursement policies
Failure to follow these rules can result in delayed payments or claim denials.
Benefits of Outsourcing Mental Health Billing
Many therapy practices struggle to manage billing internally due to limited administrative staff. As a result, outsourcing mental health billing has become a popular solution.
Some advantages include:
Expertise in Mental Health Coding
Mental health billing specialist companies understand the unique requirements of psychiatric and therapy billing.
Reduced Claim Denials
A professional mental health billing company ensures claims are coded and submitted correctly.
Improved Revenue Cycle Efficiency
Outsourced billing for mental health helps practices maintain consistent cash flow.
More Time for Patient Care
Therapists can focus on treatment rather than administrative tasks.
Scalable Billing Support
As a practice grows, outsourcing mental health billing and coding allows billing operations to scale without hiring additional in-house staff.
Choosing the Right Mental Health Billing Company
Selecting the right partner is essential for efficient billing management. Many billing companies for mental health offer specialized services tailored to therapists and behavioral health clinics.
When evaluating a provider, consider the following factors:
Experience in Behavioral Health
The best mental health billing company should have extensive experience handling psychiatric and therapy claims.
Credentialing Support
A reliable mental health billing services company should assist with therapist credentialing and insurance enrollment.
Transparent Pricing
Some providers offer affordable solutions, including options like a cheap outsource mental health billing company while maintaining service quality.
Technology Integration
Modern mental health billing solutions should integrate with electronic health record systems for streamlined workflows.
Compliance and Security
Billing services must comply with HIPAA regulations and maintain patient data confidentiality.
Services Offered by Mental Health Billing Providers
Professional billing services for mental health clinics typically include a wide range of administrative and revenue cycle functions.
Common services include:
Insurance verification and benefit checks
Coding and billing for mental health services
Claims submission and tracking
Payment posting and reconciliation
Denial management and appeals
Patient billing and collections
Credentialing and provider enrollment
These services help ensure that billing for mental health providers is accurate, compliant, and efficient.
How Outsourced Billing Improves Practice Revenue
Financial stability is critical for mental health clinics and therapy practices. Partnering with the best mental health billing services can significantly improve financial outcomes.
Reduced Administrative Costs
Outsourcing eliminates the need to hire and train in-house billing staff.
Faster Claims Processing
Experienced billing teams submit claims quickly, reducing payment delays.
Higher Clean Claim Rate
Top mental health billing company providers maintain high claim acceptance rates.
Better Compliance
Professional billing teams stay updated with payer policies and coding changes.
Improved Financial Reporting
Practices receive detailed revenue reports to monitor performance.
These benefits make outsourcing mental health billing an effective strategy for therapists who want to maintain financial stability while focusing on patient care.
Challenges Faced by Mental Health Practices Without Professional Billing Support
Practices that manage billing internally often encounter several operational difficulties.
Limited knowledge of coding updates
Frequent claim denials due to documentation errors
Delayed payments from insurance providers
Administrative workload affecting patient care
Difficulty managing insurance credentialing
Working with the best outsource mental health billing and coding services can help eliminate these challenges and improve operational efficiency.
Role of Credentialing in Mental Health Billing
Credentialing is a critical step for therapists who want to accept insurance. Without proper credentialing, providers cannot submit claims for reimbursement.
Mental health billing and credentialing services typically assist with:
Insurance provider enrollment
NPI registration and updates
Contract negotiations with insurance companies
Credentialing documentation management
By working with experienced mental health medical billing professionals, therapists can avoid credentialing delays and begin receiving payments faster.
Technology and Automation in Mental Health Billing
The healthcare industry is increasingly adopting technology to improve billing efficiency. Modern billing services for mental health integrate advanced tools that streamline the billing process.
Electronic claim submission
Automated eligibility verification
Real-time claim tracking
Revenue analytics dashboards
These innovations allow mental health billing services to deliver faster reimbursements and reduce administrative errors.
Why Specialized Billing Expertise Matters
General medical billing companies may not fully understand the complexities of therapy and psychiatric billing. This is why many practices choose mental health billing specialist companies that focus exclusively on behavioral health.
Specialized expertise ensures accurate coding, faster claims processing, and better compliance with payer policies. A trusted mental health billing services company can act as a long-term partner in managing financial operations.
How Professional Billing Services Support Mental Health Practices
Therapists and behavioral health clinics benefit significantly from working with a dedicated billing partner. Professional teams handle every aspect of billing mental health services, from claim creation to reimbursement tracking.
Many organizations rely on providers that offer comprehensive behavioral and mental health billing services designed specifically for psychiatric practices and therapy clinics.
Companies like 247 Medical Billing Services provide end-to-end support including medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services. These integrated solutions help therapists streamline billing processes, improve claim acceptance rates, and maintain steady revenue growth.
Conclusion
Billing for mental health therapists requires specialized knowledge, accurate coding, and strong compliance with insurance regulations. From eligibility verification to claim submission and denial management, every step of the billing process plays a vital role in maintaining financial stability for therapy practices.
With the growing demand for behavioral health services in the United States, many therapists are turning to professional billing partners for support. Working with experienced mental health billing companies allows providers to reduce administrative burdens, improve reimbursement rates, and focus on delivering quality care to patients.
By leveraging advanced mental health billing solutions and expert billing teams, therapy practices can ensure long-term operational success while navigating the complex world of insurance billing.
Frequently Asked Questions
What is billing for mental health therapists?
Billing for mental health therapists refers to the process of coding, submitting, and managing insurance claims for psychotherapy, counseling, and psychiatric services provided to patients.
Why is mental health billing different from regular medical billing?
Mental health billing involves session-based CPT codes, therapy documentation requirements, and strict insurance policies, making it more specialized than standard medical billing.
Should therapists outsource mental health billing?
Many practices choose outsourcing mental health billing because it improves claim accuracy, reduces denials, and allows therapists to focus more on patient care.
What services do mental health billing companies provide?
Most mental health billing services include insurance verification, coding, claims submission, denial management, payment posting, and credentialing support.
How can therapists choose the best mental health billing services company?
Therapists should look for experienced billing providers with behavioral health expertise, transparent pricing, strong compliance practices, and advanced billing technology.
Kategorien
- Lifestyle
- Motivation
- News & Trends
- AI
- Gadgets & Reviews
- Tech News
- Marketing
- Ausbildung
- Health & Fitness
- Travel
- Food & Cooking
- Entertainment
- Home & Living
- Sports
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- Spiele
- Gardening
- Health
- Startseite
- Literature
- Music
- Networking
- Andere
- Party
- Religion
- Shopping
- Sports
Mehr lesen
https://xn----jtbtibrbj7a4dza.xn--p1ai/reeltor55 https://nwacolorado.org/author/reeltor53/ https://drummitup.com/drummitup-member.php?action=profile&uid=224749 https://studycrafter.com/studycrafters/reeltor55/ https://www.sqlservercentral.com/author/reeltor53 https://buymusicclub.vercel.app/user/reeltor00 https://paperpage.in/reeltor55...

Introduction to Jumbolon Sheet in Pakistan in Modern Building Materials Jumbolon sheet in Pakistan has become a widely used material in the construction industry due to its lightweight structure and insulation properties. It is made from expanded polystyrene which creates a foam based sheet with excellent performance characteristics. Jumbolon sheet in Pakistan is commonly used in roofs...

The King Sp5derr T Shirt is becoming a popular choice for people who want comfort and style together. These T shirts are designed to move with your body, making them perfect for everyday activities. Whether you are walking, commuting, or hanging out with friends, the fabric and cut of King Sp5derr T shirts allow easy movement. Many streetwear fans prefer clothing that does not restrict their...

The excitement around early-stage crypto investments continues to grow, and many investors are asking the same question: Are presale coins actually worth it? A crypto presale coin offers investors the opportunity to buy tokens before they are publicly listed on exchanges — often at a discounted price. While the potential upside can be attractive, the risks are equally significant....

The global Mass Spectrometer Market is undergoing significant transformation, driven by advancements in analytical technologies, rising R&D investments, and expanding applications across industries such as pharmaceuticals, biotechnology, environmental monitoring, food safety, and clinical research. GLOBAL SUPPLY CHAIN DISRUPTION ALERT Escalating tensions around the Strait of Hormuz and...



